
Blog - PEM ED Podcast
Andrew Sloas
- HEMOPHILIA EMERGENCIES

Tara's kids...doing all the same things other kids do!!!
A while back now, I got an email from Weingart stating that he had received correspondence form a Canadian paramedic by the name of Tara Anema. Tara really wanted to get the word out about a particular pediatric patient population that she had seen mismanaged by all levels of emergency provider in all types of situations. Why all the hubbub about this particular group…well the condition is hemophilia and her own two sons are effected. After speaking to Tara I knew her passion and message was perfect for the show. I have also brought in our hemophilia expert from the University of Kentucky, Dr. Vlad Radulescu to answer all your burning questions about how we SHOULD be taking care of these children.
As a bonus this month, stay tuned to the end of the show when Dr. Marianne Gausche-Hill and I do a little update on Pediatric Readiness and be sure to check out her most recent publication below!!
http://www.pediatricreadiness.org/
JAMA PEDIATRIC READINESS ARTICLE JUNE 2015ACEP Policy Statement on the Care of Children in Emergency Departments
BASICS OF EMERGENCY MEDICINE POCKET GUIDE
BASICS OF EMERGENCY MEDICINE: PEDIATRIC POCKET GUIDE
 13 July 2015, 2:27 am
13 July 2015, 2:27 am - Pediatric Syncope Part Deux...Still Fell Out
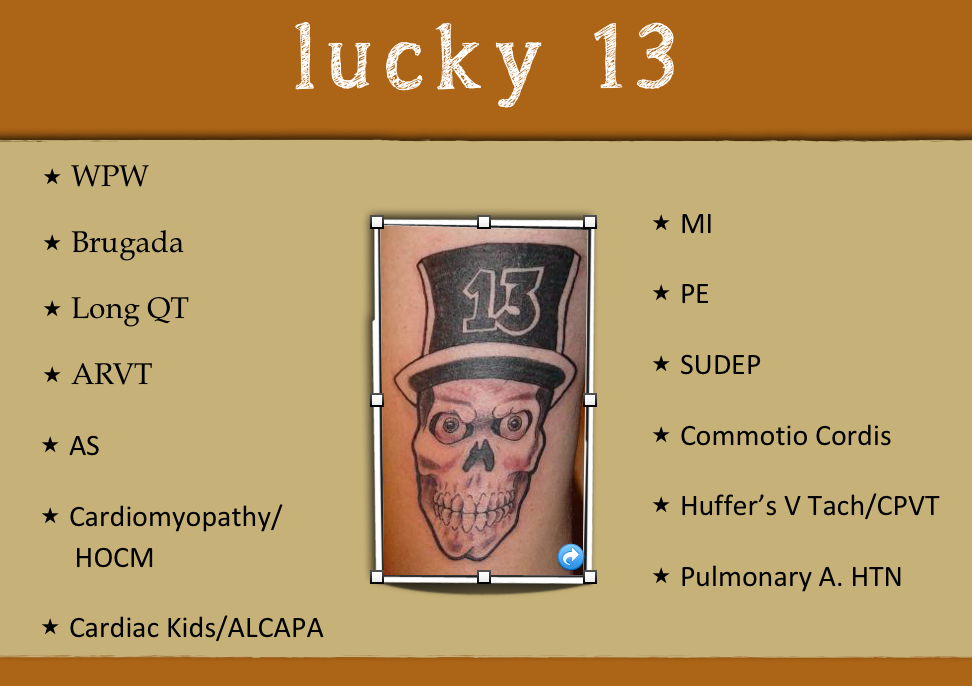
Buck Kyle MD...AKA pediatric cardiologist extraordinaire... is back to finish up part two of our in-depth look at pediatric syncope and the thirteen causes of sudden cardiac death. Never feel threatened by the patient with a chief complaint of DFO (done fell out) again! For the next hour we will cover the rest of the electrical, structural, and miscellaneous conditions that are responsible for V Tach/DFO, which may can ultimately to sudden cardiac death.
Pediatric Syncope and POC Echo Article
Pediatric ECG Cardiomyopathy 8mm Q-wave lead III
 25 April 2015, 6:36 pm
25 April 2015, 6:36 pm - Best Case Ever and Ask Me Anything
I was recently asked to discuss my best case ever with Anton Helman, MD of Emergency Medicine Cases and then to join Alex Koyfman, MD from EMDocs for a session of "Ask Me Anything." Both were so much fun and we covered a lot of interesting material. You have to check out these two sites they are fantastic!!! Thanks to both for the invites!!!
Click the links below:

 8 February 2015, 6:44 am
8 February 2015, 6:44 am - Pediatric Syncope (DFO ~ Done Fell Out)
Welcome back to the show Dr. Buck Kyle! Dr. Kyle is a attending pediatric cardiologist at Texas Children’s Hospital and on this episode we will discuss what causes all those little kids to pass out before they come to your ER and then look so fantastic. Are they all OK to go home? Is there anyone in there that’s truly sick and if so how do we identify that subset? Sit back, hold on tight, and try not to DFO (done fell out) because it’s going to be fast, fun, and may leave you a little mareado….

Long QT Medication Website
 4 February 2015, 3:07 am
4 February 2015, 3:07 am - The Five Canons of Levitan - Difficult Airway Part 3
Canon - a general law, rule, principle, or criterion by which something is judged
No one has changed the face of how we approach difficult airway more than Rich Levitan, MD. In this episode I review five of Rich's most important contributions to how we approach emergent intubations. These are techniques you can take to the department tomorrow to improve your view, increase your success, and save your patient's life!

Click here to follow Dr. Levitan on twitter.
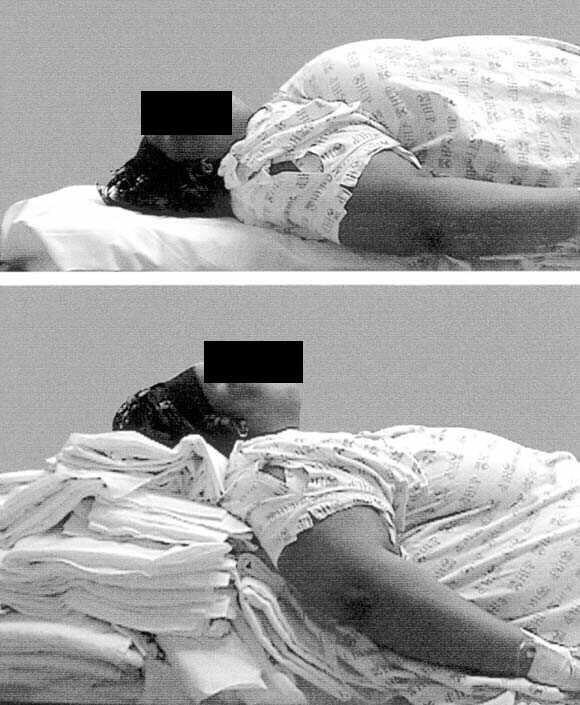
Ear to sternal notch positioning will not only improve your view, but save your backside and possibly your patient's life!
Levitan's best bougie techniques (includes Shaka, Kiwi and Ducanto)!


 2 December 2014, 7:22 am
2 December 2014, 7:22 am - Child Abuse

It is hard to put into words or even imagine the concept of someone intentionally hurting a child, but it happens more frequently than we'd like to believe. In this episode, I had the privilege of discussing some of the cornerstone exam findings and history flags for occult abuse with Marci Donaruma-Kowh, MD a child abuse expert from the Baylor College of Medicine ~ Texas Children's Hospital. This episode will change the lens you view your pediatric patients through; even with those who have what appears to be the most mundane of injuries. Unfortunately, abuse is not always overt and Dr. Donaruma is an expert in identifying the subtleties of this diagnosis, nailing the perpetrator, and making sure they go away for a long-long time...
If you know of a child that is being abused call the police now. If you would like to refer a case and you are in the Houston area please click here: Children's Assessment Center.
16 October 2014, 2:18 am - Asthma and the Vent

TOP = AUTO PEEP BOTTOM = NORMAL FLOW
Set the Vent in SIMV at 7cc/kg and an I:E ratio of 1:4/1:5 and check a blood gas! — Andrew Sloas, DO, RDMS, FAAEMWow! We've made it to the end of three episodes on asthma. We've covered everything from diagnosis to treatment and everything in between. We now know how to best educate our patients to empower them to treat their disease at home and prevent recitivism!
Tune in this episode for the specifics on how to use a Peak Flow Meter, Bi-Pap, EtCO2 and of course how to set-up the ventilator in a way to maximize support and minimize chances of injury in your asthmatics.
EM Crit - Infamous Awake Sedated Video
EM Crit - Dominating the Vent Part 1
EM Crit - Dominating the Vent Part 2




 26 August 2014, 6:16 am
26 August 2014, 6:16 am - Asthma Andrews Style - What's the best oral steroid you ask?

What's the best oral steroid to treat acute asthma exacerbations you may ask? Well, we're here to answer that for you. Please welcome Dr. Annie Andrews, MD, MSCR who has written all the articles you will find listed below on just that subject. In this podcast we will prove that dexamethasone is not only the most cost effective steroid to prescribe in asthma exacerbations, decreases recidivism, and has the best compliance rates, but it tastes great too!
http://www.paramedictorn.org/trauma-care.html
Andrews AL, Simpson AN. Dexamethasone may be a viable alternative to
prednisone/prednisolone for the treatment of acute asthma exacerbation in the
paediatric emergency department. Evid Based Med. 2014 Jun 10. pii:
ebmed-2014-110006. doi: 10.1136/eb-2014-110006. [Epub ahead of print] PubMed
PMID: 24919976.
Andrews AL, Wong KA, Heine D, Scott Russell W. A cost-effectiveness analysis
of dexamethasone versus prednisone in pediatric acute asthma exacerbations. Acad
Emerg Med. 2012 Aug;19(8):943-8. doi: 10.1111/j.1553-2712.2012.01418.x. Epub 2012
Jul 31. PubMed PMID: 22849379.
Keeney GE, Gray MP, Morrison AK, Levas MN, Kessler EA, Hill GD, Gorelick MH, Jackson JL. Dexamethasone for acute asthma exacerbations in children: a meta-analysis. Pediatrics. 2014 Mar;133(3):493-9. doi: 10.1542/peds.2013-2273. Epub 2014 Feb 10. Review. PubMed PMID: 24515516; PubMed Central PMCID: PMC3934336.
1 July 2014, 8:10 am - Asthma...The Music Of The Night

In this episode, the first of a three part series on asthma, we will cover the diagnostic and treatment strategies that will help you rapidly move patients through your ED. No, of course you don't need the patient's asthma classification, but you DO NEED to understand which patients need more treatment and when it's OK to stop. I will break that all down for you with the aid of the algorithm above. We'll talk in depth about who can go home safely and who should be in the Unit! Download the flow sheet from the link above, put it in your smart-phone so you have it for your next asthma encounter, and follow along. It's going to get musical..

Rich Levitan's Yellowstone Advanced Airway Critical Care Course

Cabo CME Course - Levitan, Weingart, Matt & Mike, Orman, and Sloas
24 May 2014, 7:07 am - Anyone Seen My Corn? Pediatric Foreign Bodies

THE DERMA-Q
How many times have you seen a square object inserted into a round hole.....of an ear canal??? It's quite a quandary and can be the source of frustration for both you and the patient. You may end up waiting two to three hours just to be able to sedate the little bugger because they have usually just choked down a cheese burger and fries (if your in Britain it may be bangers and mash, Australia a vegemite sandwich, Russia borscht, etc, etc) and then even after you have them sedated, you don't have the right tool to get the foreign body out because the right tool was never created… that is, until now! Thanks to Dr. David DeLemos from the Texas Children's Pediatric Emergency Medicine program, we now have the solution to the round (or square) object in the ear canal. Let me be the first to introduce you to the "Derma-Q." The Derma-Q is a contraption created from the plunger of a small syringe or a Q-tip, which has then been tipped (like a tribal dart) with a minute amount of Dermabond. The Derma-Q provides the perfect rescue technique to get those tough foreign bodies out of almost any orifice. Also making her debut this month on the PEM ED Podcast, my wife, Dr. Holly Sparks will risk life, limb, and my ear canal by getting a cheap piece of plastic jewelry out of my EAC for your viewing pleasure.
Rich Levitan's Yellowstone Advanced Airway Critical Care Course
Cabo CME Course - Levitan, Weingart, Matt & Mike, Orman, and Sloas
9 April 2014, 4:24 am - Are You Ready...For Little Patients?

Dr. Facilier begged the question..."Are you ready for Transformation Central?" Transformation? My ER runs just fine. What could I need to be ready for or transform my ER into??? Well, there's this little thing standing between you and poop in your underwear; most of us call them pediatric patients. What should scare you is that 30% of the hospitals in the US are not ready and by not ready I mean that they do not have the proper equipment or training necessary to take care of critically ill patients. So I say again, ask yourself, what is the most stressful patient whom you to take care? Is it the little old urosepsis patient that needs an art line, central line and intubation or the neonate that needs the same procedures. OK, the procedures are stressful, but what if you don't have the equipment to to do them. Do you know if your ER stocks a size 1 LMA? Now's the time to figure it out, not once the patient is staring you in the face (probably wide eyed). This month we are fortunate enough to be joined by the esteemed Dr. Marianne Gausche-Hill who is the creator and lead investigator on the Pediatric Readiness Project. We now know from a decade of research that 30% of hospitals in the US are missing the equipment needed to take care of these patients do you work at one of those????
http://www.pediatricreadiness.org/
Dr. Gauche Hill would like to thank: Dr. Kate Remick, The Federal EMS for Children Program Director Elizabeth Edgerton, National EMS for Children Data Analysis and Resource Center, American College of Emergency Physicians, American Academy of Pediatrics, the Emergency Nurses Association, State of California EMS Authority, and all the EMS for Children’s Coordinators in the US and its territories.
ACEP Policy Statement on the Care of Children in Emergency Departments
Rich Levitan's Yellowstone Critical Care Airway Course - May/June 2014
See you in CABO!!! The new Podcaster's CME conference put on by EB Medicine:
Cabo CME Course - Levitan, Weingart, Mike & Matt, Orman and Sloas
9 February 2014, 6:17 pm - More Episodes? Get the App
Your feedback is valuable to us. Should you encounter any bugs, glitches, lack of functionality or other problems, please email us on [email protected] or join Moon.FM Telegram Group where you can talk directly to the dev team who are happy to answer any queries.
 Academic Life in Emergency Medicine (ALiEM) Podcast
Academic Life in Emergency Medicine (ALiEM) Podcast
 Pediatric Emergency Playbook
Pediatric Emergency Playbook
 Emergency Medicine Chapter Summary Podcast
Emergency Medicine Chapter Summary Podcast
 Emergency Board Review
Emergency Board Review
 PEM Currents: The Pediatric Emergency Medicine Podcast
PEM Currents: The Pediatric Emergency Medicine Podcast
 TamingtheSRU
TamingtheSRU